| |
Circumcision and Breast-feeding
There is scientific evidence
that the trauma of circumcision
makes it harder for a baby
to learn how to suckle.

L M D
| |
Upon my lap my sovereign sits
And sucks upon my breast;
Meantime his love maintains my life
And gives my sense her rest.
Sing lullaby, my little boy,
Sing lullaby, mine only joy!
- English lyric.
|
T-shirts and mugs now available
with an attractive tinted
version of this image

from The Intactivism Shop.
Birth-recovery disrupted:
Dixon et al compared three groups of babies: circumcised with anaesthesia, with a saline injection to simulate the trauma of injection alone, and with no anaesthetic. (They did not leave a control group intact.) After giving the babies a standard test of a variety of behaviours, they concluded:
|
"This report adds to the growing body of data that indicate that circumcision is a painful procedure that disrupts the course of behavioral recovery following
birth."
|
Sleep disrupted:
Emde et al. found:
|
"Routine circumcision, done without anesthesia in the
newborn nursery was usually followed by prolonged
nonrapid eye movement (NREM) sleep. Since this form
of sleep has been described as a low point on an arousal
contin[u]um, we consider its increase to be consistent
with a theory of conservation-withdrawal in response to
stressful stimulation."
|
Behaviour disrupted:
Marshall et al. conducted a standard battery of tests (the Brazelton Neonatal Behavioral Assessment Scale, or NBAS) on two groups of babies, one circumcised at two days, the other at three weeks, with the experimenters kept ignorant of the circumcision status of the babies. They found:
|
"...our results demonstrate tha[t] infants change
behaviors after circumcision in about 90 percent of cases."
|
Feeding disrupted: Marshall et al. also observed mother-infant interaction in two groups of 29 babies at the same times over three days after birth, one group circumcised on the second day, the other after all four observations were complete. The babies were all bottle-fed, however. The mothers were supposedly kept ignorant as to whether their babies had been circumcised yet.
| "... immediately following circumcision there were differences in the feeding patterns between the two groups. The experimental [circumcised] group exhibited fewer intervals of uninterrupted feeding than did the control [not yet circumcised] group. ... subjective descriptions support the observations that the infants who were circumcised sucked on the bottles harder, faster and more concertedly."
|
Breast-feeding disrupted:
Howard et al conducted a "prospective, randomized, double blind, placebo-controlled, clinical trial of acetaminophen analgesia in 44 healthy full term neonates undergoing circumcision...." (They did not have an intact control group.) "Beginning two hours before Gomco circumcision, neonates received either acetaminophen...or placebo...." They found that:
|
"Neonates in both groups showed significant increases in heart rate, respiratory rate, and crying during circumcision with no clinically significant differences between the groups. Postoperative comfort scores showed no significant differences between the groups until the 360-minute postoperative assessment, at which time the acetaminophen group had significantly improved scores.... Feeding behavior deteriorated in breast- and bottle-fed infants in both groups, and acetaminophen did not seem to influence this deterioration."
|
Routine infant circumcision (RIC) became fashionable in the English-speaking world this century at the same time as the rise of bottle-feeding from birth, so any ill-effect of circumcision on the suckling reflex would not have been noticed. (Jewish ritual circumcision might not have this effect, because the baby would have had a week to bond with his mother and learn the suckling interaction before he was circumcised.)
The AAP:
In December 1997, the American Academy of Pediatrics published a policy on Breast Feeding and the Use of Human Milk which said
|
"Breastfeeding should begin as soon as possible after birth,
usually within the first hour. Except under special circumstances,
the newborn infant should remain with the mother throughout
the recovery period. Procedures that may interfere with breastfeeding or traumatize the infant should be avoided or minimized."
|
...but did not mention circumcision directly. This passage is missing from its 2012 policy. The nearest it now comes is:
...emphasis is placed on the need to revise or discontinue disruptive hospital policies that interfere with early skin-to-skin contact, ... that restrict the amount of time the infant can be with the mother...
|
In 2001, the AAP's Committee on Psychosocial Aspects of Child and Family Health, along with the American Pain Society's Task Force on Pain in Infants, Children, and Adolescents, issued a Policy Statement , which says
Local anesthetics and strategies to soothe and minimize distress should be considered even for simple procedures, such as venipuncture. Some common painful minor procedures, such as circumcision, do not always receive the warranted attention to comfort issues. Available research indicates that newborn circumcisions are a significant source of pain during the procedure and are associated with irritability and feeding disturbances during the days afterward.9-11 Opportunities for alleviating pain exist before, during, and after the procedure, and many interventions are effective.12-17 |
- "The Assessment and Management of Acute Pain
in Infants, Children, and Adolescents" (0793)
Pediatrics, Volume 108, Number 3, September 2001, pp 793-797
...but of course, the most effective intervention, and the greatest opportunity for alleviating pain (completely) exists instead of the procedure: saying No to circumcision.
Anecdotal evidence:
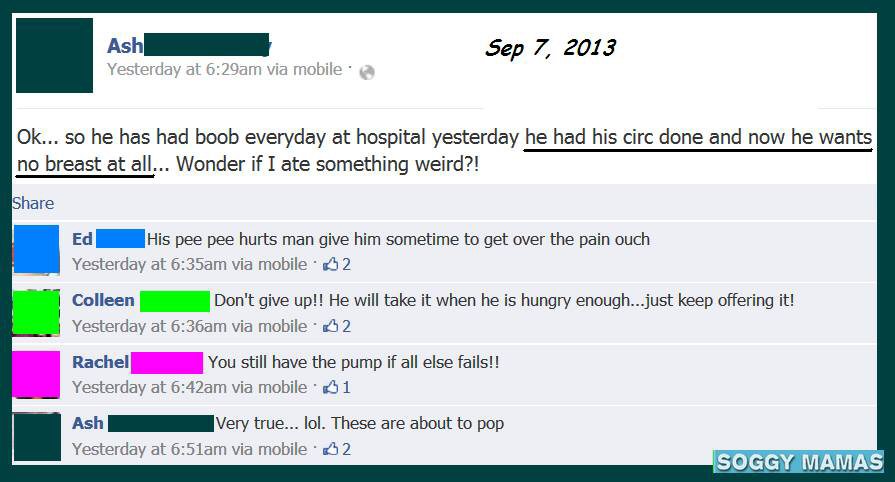
A nurse with 19 years experience with nursing mothers writes:
|
Breastfeeding is often irreparably damaged by circumcision. At the time of most circumcisions, many mothers and babies are barely getting the hang of breast feeding and the baby is sometimes literally torn off the breast for his journey to the circ room. When he comes back, he is often in shock, in a deep sleep, and unarousable, or so irritable that he is inconsolable and will not take the breast, making the offer of a bottle by a healthcare professional more likely to be accepted. The main thing with getting breastfeeding going is uninterrupted exposure of baby to mother. They are one. Anything not crucial to sustaining life should be avoided. This is a huge concern in the pro-breastfeeding community.
|
|
Hartford Courant
August 18, 2002
Back In The Mouths Of Babes
There's A Movement To Put Breasts Back Where They Belong...
August 18, 2002
By Charlotte Meryman, Northeast Magazine
...
Fair-skinned and freckled, with shoulder-length, blond hair, [Debra]
Kronschnabel, 35, settles into a large, upholstered nursing chair,
unbuttons her denim shirt, unhooks the front of her nursing bra, and
brings (newborn twin boy) Erich to her breast. She is skeptical of the
effort. In the couple of hours since their last nursing session, Erich was
circumcised, and he is so exhausted from crying that Kronschnabel knows
even the scent of his mother and the feel of her nipple against his mouth
are unlikely to rouse him.
But [Dr. Kathleen] Marinelli has a lot of tricks in her bag. Leaning over the chair
facing Kronschnabel, she tickles Erich's feet and sides, and loosens his
clothing in an effort to disturb [!] him. Then she lifts him away from the
swaddling comfort of his mother's body. Finally, she passes him back to
the attending nurse, Laura Miele, who removes the IV needle still taped to
the back of his right hand. As Miele peels the tight adhesive, Erich
finally begins to cry. His mouth open wide in a scream, he is passed back
to his mom and latches on immediately. The nipple in his mouth is all the
comfort he was looking for, however, and soon he drifts back to sleep.
Marinelli directs Kronschnabel to squeeze out some milk by gently
compressing her breast with her thumb and fingers, but even the taste of a
meal has no effect on Erich. Normally, such a sleepy baby [He's not sleepy, he's in shock] would be left
alone until he is ready to nurse, but Marinelli can't afford to do that
with Erich, who must keep up his food intake. So she switches to plan B.
She sends Figueroa to the other side of the room to fetch Klarissa (the
female twin), with the hope that her suckling will create the milk letdown
needed to get Erich going. Again, Kronschnabel is doubtful. Klarissa
nursed until she was full just an hour ago.
Marinelli proceeds anyway, helping Kronschnabel position Klarissa at her
right breast, with Erich on the left and soon both are exhibiting the
long, drawing sucks and swallows that indicate real eating. Kronschnabel
is amazed. "I didn't think we were going to get him to go."
...
So the bottom line seems to be, if you want to circumcise and breastfeed - have twins (one a girl).
|
UTIs:
There is also evidence that breastfeeding colonises the baby's body with the mother's benign bacteria, and so indirectly helps protect him (or her) against urinary tract infections (UTIs), one of the main, if most recent, excuses for circumcision.
Pisacane et al. found artificially-fed babies were more than 2½ times as likely to suffer UTIs as breastfed babies:
|
"Compared with infants who were bottle fed, breast-fed patients had a
relative risk of UTI of 0.38 (95% confidence intervals 0.22 to 0.65) when a
dichotomous classification (ever breast fed vs never breast fed) was used."
|
This is confirmed by the study of Marild et al:
Acta Paediatr. 2004 Feb;93(2):164-8.
Protective effect of breastfeeding against urinary tract infection
Marild S, Hansson S, Jodal U, Oden A, Svedberg K.
Department of Paediatrics, The Queen Silvia Children's Hospital,
Sahlgrenska University Hospital, Goteborg, Sweden.
staffan.marild@pediat.gu.se
AIM: To assess the possible protective effect of exclusive breastfeeding
against first-time febrile [feverish] urinary tract infection (UTI) in children.
METHODS: Two children's hospitals and local child health centres in the
Goteborg area, Sweden, participated in a prospective case-control study.
In total, 200 consecutive cases (89M, 111F), aged 0-6y, presenting with
first-time febrile UTI were enrolled. The mean +/- SD age was 0.98 +/-
1.15 y. As control subjects, 336 children (147M, 189F) were recruited from
the child health centre of the case, matched for age and gender and
included consecutively for each case during the first days after
diagnosis. The duration of exclusive breastfeeding was obtained from the
case and controls by a standardized procedure.
RESULTS: Ongoing exclusive
breastfeeding gave a significantly lower risk of infection. A longer
duration of breastfeeding gave a lower risk of infection after weaning,
indicating a long-term mechanism. The protective role of breastfeeding was
strongest directly after birth, then decreased until 7 mo of age, after
which age no effect was demonstrated.
CONCLUSION: A protective role of
breastfeeding against UTI was demonstrated. The study provides statistical
support to the view that breast milk is a part of the natural defence
against UTI.
PMID: 15046267 [PubMed - indexed for MEDLINE]
[NB Virtually none of these Swedish babies would have been circumcised.]
|
Painkillers:
The AAP recommends that local anaesthetic be used with circumcision, but ...
|
Painkillers disrupt infant bonding
LONDON, March 28, 2001(Reuters)
- Painkillers given to women during childbirth could be preventing mothers from bonding with their babies, New Scientist magazine said on Wednesday.
Scientists at the Karolinska Institute in Sweden videotaped 28 newborns to
see how they responded to their mothers, some of whom had pain relief.
"We wanted to see how interventions like analgesia affect a newborn's
behaviour," said Anna-Berit Ransjo-Arvidson who conducted the study.
All of the infants were cleaned and placed on their mother's breast. The
infants not exposed to the drugs behaved normally and reached for their
mother and began to feed about an hour after birth.
But the babies of mothers who had taken painkillers did not interact as much
with their mother and took longer to feed.
Levels of the hormone oxytocin, which controls lactation and the contraction
of the uterus and is thought to increase bonding, rose in women without
painkillers when their babies fed.
The Swedish scientists suspect that because babies exposed to painkillers
interact less with the mother there is less oxytocin released and the two do
not bond as well.
"We need to do more studies, especially as there is a very high increase in
(the use of) epidural and other pain relievers," said Ransjo-Arvidson.
"There's a lot of money in epidurals," she added.
|
[And that's only when the babies receive the painkillers indirectly, through the placenta before birth. How much more so when they are themselves directly injected with the painkillers...]
Bottle feeding
Nobody has ever suggested that circumcision interferes with bottle feeding. There are several salient differences from breast feeding:
- The baby must suck harder to draw milk from the breast than from a bottle.
- The baby must be nestled in to the mother to breastfeed, pressing a circumcision wound against her body and causing him additional pain
- Breast feeding benefits from a calm state of mind in both mother and baby, as bottle feeding does not.
- The breast feeding relationship develops between mother and baby in the first few days of life: bottle feeding may be purely nutritive.
So it is hardly surprising that a study of babies who were all bottle fed shows no difference before or after circumcision. (The study did not have a control group of babies who were not circumcised at all.)
|
Hosp Pediatr. 2013 Oct;3(4):362-5. doi: 10.1542/hpeds.2012-0082.
Neonatal circumcision: is feeding behavior altered?
Gattari TB, Bedway AR, Drongowski R, Wright K, Keefer P, Mychaliska KP.
Abstract
BACKGROUND:
The effect of circumcision on feeding behavior in the newborn period
is unknown. We hypothesized that circumcision would not have a
significant effect on newborn feeding.
METHODS:
This prospective study analyzed the effect of circumcision on
neonatal feeding behavior. Inclusion criteria were healthy male
infants who were exclusively bottle-fed and underwent a circumcision
before discharge from the newborn nursery. We collected data (N =
42) on gestational age, birth weight, Apgar scores, maternal age,
gravid status, anesthesia used during delivery, analgesia used after
circumcision, time of circumcision, and volume and frequency of
feeding before and after circumcision. Data were analyzed by using
paired t tests, multivariable regression analysis, and analysis of
variance (with SPSS version 18). Significance was P < .05 (2-tailed
α).
RESULTS:
Descriptive statistics for the entire group (N = 42) are as follows:
mean ± SD gestational age: 38.7 ± 1.2 weeks; mean birth weight:
3.3 ± 0.4 kg; maternal age: 26.7 ± 6.3 years; baseline feeding
(mean of first 2 feedings before circumcision): 24.5 ± 9.9 mL; mean
first feeding after circumcision: 21.7 ± 11.9 mL; and mean second
feeding: 26.7 ± 13.5 mL. Forty-eight percent of patients increased
their feeding volume after circumcision compared with baseline, and
52% of patients decreased their feeding volume, which persisted with
the second feeding. There was no statistical difference between the
baseline and first feeding (P = .11) or second feeding (P = .22).
CONCLUSIONS:
Our data suggest that circumcision does not alter [bottle] feeding after
circumcision. This information will be useful in counseling families [who intend only to bottle feed]
regarding circumcision in the newborn period.
PMID: 24435194 [PubMed - in process]
|
The design of this study almost suggests that it was meant to muddy the water so that circumcision advocates could say "It has been scientifically shown that circumcision has no effect on feeding" and let people assume that meant breast feeding.
La Leche:
The La Leche League refuses to take a stand on circumcision nowadays, claiming it is not a breastfeeding-related issue - though it takes a stand on many other issues whose relationship to breastfeeding is just as indirect, such as "co-sleeping" (sharing a bed), pacifiers, etc.
However, the Breastfeeding Answer Book says:
When a baby undergoes a painful medical procedure, such as a heel stick, injection, spinal tap, or circumcision, he may shut down and be unreceptive to feedings until he is feeling better.
|
The League's handbook, "The Womanly Art of Breastfeeding" said in its 1981 edition:
|
ELECTIVE SURGERY FOR YOU OR BABY
[No baby "elects" circumcision.]
If you are going to be in the hospital anyway for the birth of your
baby, you or you doctor may suggest that you have some other medical
matter attended to. Examples of elective surgery for the mother include
stripping the legs of varicose veins or tying the fallopian tubes (tubal
ligation). As for the baby, it may be considered almost routine to
circumcise boy babies when they are only a few hours or days old. But
circumcision is an elective surgery and you have a choice of whether or
not to have your baby circumcised. You can also choose to wait a while before having this done. We bring these subjects up because, physically and emotionally, these procedures all take their toll on mother and child. Since they represent elective surgery, their appropriateness at this critical time must be questioned.
Circumcision is as painful a procedure to a newborn as it is to an
adult. As a religious rite, circumcision is not performed until the baby
is eight days old, when he is less apt to hemorrhage. The reasons given
in the past for non-religious, almost routine circumcision of the
newborn were generally hygienic and are no longer accepted by many
physicians and parents. If you're interested in learning more about this
subject, see the Book List at the end of this book.
The most important reason for siding against elective surgery following
childbirth is that it interferes with a mother and her new baby being
together and getting to know each other. While a mother may feel very
good following the birth of her baby, her body nevertheless has some
recovering to do. Adding the strain of recovering from a surgical
procedure might lessen her enjoyment of these early days with her baby.
In regard to tubal ligation, there can often be an unexpected emotional
reaction in the mother. When it dawns on her that the baby in her arms
is her last, there may be feelings of deep sadness. It might become
difficult for her to keep a normal perspective on her mothering of this
baby. She may become exceeedingly anxious about doing everything just right.
Whatever the inconvenience you may experience by postponing such
operations for you or your baby, it is slight compared to the upheaval
such surgery can cause in your life at this time."
[pp 92-3]
from the League's book list, in the section called Prenatal Care and Childbirth:
"Circumcision: An American Health Fallacy" by Edward Wallerstein
Springer Publishing: 1980. Softcover.
Available from Birth & Life
A very definitive book, covering twelve years of research. The author
feels like circumcision is a solution in search of a problem. Extensive
arguments against routine circumcision are presented in a most readable
manner.
[p.350]
|
The Mother-Friendly Childbirth Initiative:
The
Mother-Friendly Childbirth Initiative "discourages non-religious circumcision of the newborn."
(There is also a
more easy-to-read version.)
The preamble
includes the statement "Current maternity and newborn practices that
contribute to high costs and inferior outcomes include the inappropriate
application of technology and routine procedures that are not based on scientific evidence."
The organization that put the initiative together is The Coalition for Improving
Maternity Services [CIMS, pronounced "kims"], which represents more
than 90,000 birth professionals.
CIMS grant permission "to freely reproduce this
in whole or in part along with complete attribution.
Please email our webmaster if you place this
on your site so we can inform you of updates."
This initiative was ratified by La Leche
League in July 1996 and the International Lactation Consultant
Association, among other organizations.
Another resource:
The Lactivist-Intactivist site unites the campaigns for breast-feeding and against circumcision.

A summary of this page may be downloaded as a Word document or in .pdf format (which requires Adobe Acrobat Reader ).
| "Impact of Birthing Practices on Breastfeeding: Protecting the Mother and
Baby Continuum" by Mary Kroeger with Linda J. Smith. Jones and Bartlett
Publishers, 2003, pp 197-198.
"According to the Council on Scientific Affairs of the American Medical
Association, circumcision is a non-therapeutic procedure without
documented benefit for the infant. Hill has raised concerns in a letter
to a lactation journal about how little the matter of possible negative
effects on breastfeeding from circumcision is addressed in the
literature or in parental counseling. Circumcision is a traumatic and
painful procedure that induces hard crying and that will continue to
cause postoperative pain to the newborn. Anesthetic is used in less than
half of the procedures done, according to one survey. This is despite
the fact that the American Academy of Pediatrics (AAP) has called for
the use of anesthetic.
In his letter, Hill notes 25 years of studies documenting breastfeeding
difficulties in infant males who have been circumcised. Howard et al.
studied 44 infants after circumcision and found less-frequent feeding
and withdrawn, subdued, less-interactive behavior. Howard cautions that
because many babies are discharged on the day the circumcision is
performed, they are lost to immediate follow-up for subsequent
breastfeeding problems. Breastfeeding newborns in this study required
supplementation due to their mother's perception that the baby could not
breastfeed or had true difficulties with feeding. Early supplementation
before the onset of lactogenesis is known to be associated with
breastfeeding failure. Given the strong arguments for protecting a calm,
safe, pain-free environment for the newborn to transition to life
outside the warmth and cushion of the uterus, Hill argues that
"successful breastfeeding should be given absolute priority over
neonatal circumcision." The work group on breastfeeding in the AAP has
also called for avoidance of painful procedures like circumcision.
Fleiss has written extensively on the initial and long-term trauma to
infants from circumcision. He writes: "The radical practice of routinely
circumcising babies did not begin until the Cold War era. This
institutionalization of what amounted to compulsory circumcision was
part of the same movement that pathologized and medicalized birth and
actively discouraged breastfeeding.
References
American Medical Association, Council on Scientific Affairs. 1999.
Report 10: Neonatal circumcision. Chicago IL: American Medical
Association.
Hill G. 2003. Breastfeeding must be given priority over circumcision.
Letter in J Human Lact 19(1):21.
Stang HJ, Snellman LW. 1998. Circumcision practice patterns in the
United States. Pediatrics 101:e5.
Marshall RE, Porter FL, Rogers AG, et al. 1982. Circumcision II: Effects
on mother-infant interaction. Early Hum Dev 7:367-374.
Howard CR, Howard FM, Weitzman ML. 1994. Acetaminophen analgesia in neonatal circumcision: The effect of pain. Pediatrics 93:641-646.
Academy of Pediatrics, Workgroup on Breastfeeding. 1997. Breastfeeding and the use of human milk. Pediatrics 100:1035-1039.
Fleiss P. 1997. The case against circumcision. Mothering Magazine Winter 1997:36-45.
|
A contrary study
|
Wiley Interscience
Neonatal circumcision: Effects on breastfeeding and outcomes associated with breastfeeding
David M Fergusson, Joseph M Boden and L John Horwood
ABSTRACT
Aim: There have been recurrent claims made that neonatal circumcision disrupts the development and maintenance of breastfeeding in infants. The aim of the current study was to use a longitudinal birth cohort study to examine the associations between neonatal circumcision status and both breastfeeding outcomes, and health and cognitive ability outcomes associated with breastfeeding.
Method: Data were obtained from the Christchurch Health and Development Study, a longitudinal study of over 1000 individuals born in Christchurch New Zealand in mid 1977. Data were obtained for male cohort members (n = 635) on circumcision status, breastfeeding outcomes, health outcomes in infancy and cognitive ability outcomes later in life.
Results: Circumcision status was not significantly associated (P > 0.05) with breastfeeding outcomes in infancy, even following adjustment for covariate factors, including maternal age, family socio-economic status, ethnicity and birthweight. Also, circumcision status was not significantly associated (P > 0.05) with health in infancy and cognitive ability outcomes in later childhood, even after adjustment for covariate factors.
Conclusions: There was no evidence of an association between neonatal circumcision status and breastfeeding outcomes, or between circumcision status and health and cognitive ability outcomes associated with breastfeeding, and the findings do not support the view that neonatal circumcision disrupts breastfeeding.
One problem with this study is that breastfeeding data was obtained from the mothers at four months, long after circumcision, and the measures of breastfeeding outcomes used were somewhat crude. (The Christchurch cohort has yielded two other sets of circumcision data, one on Sexually Transmitted Infections that got world-wide publicity far beyond its significance, and one of "penile problems" that counted circumcision complications in those circumcised post-neonatally as complications of intactness.)
|
Related pages:
A useful Guide to Breastfeeding
Back to the Intactivism index page.
The verse is quoted in "The Sources of Love and Fear" by Dr Maurice Bevan-Brown, Raven Press, Christchurch NZ, 1950, and the illustration is based on its cover. In it, Bevan-Brown also wrote - half a century ago:
Circumcision
It is extraordinary that in our day this rather barbaric rite should be practised almost as a routine with infants. From the psychological point of view it is dangerous with or without an anaesthetic. In the rare case where a child cannot urinate it may be done, but is otherwise unjustifiable. Apparently the practice is based on a morbid fear of masturbation, and it is unconsciously propitiatory. When performed at the age of two or three, it is frequently the basis of severe castration fears.
(Babies urinate in utero, and would not survive to term if they could not.)
|
Frontispiece of "The Sources of Love and Fear":
This cartoon was drawn by a patient who, with neo-Freudian Dr Bevan-Brown's help, had interpreted the ogress as his mother and the knife as a bottle. But sometimes a cigar is just a cigar, and sometimes a knife is just a knife....
References:
Suzanne Dixon, M.D., Joel Snyder, M.D., Richard Holve, M.D., Patricia Bromberger, M.D, "Behavioral Effects of Circumcision with and without Anesthesia" Developmental and Behavioral Pediatrics 1984 Vol. 5 No. 5: pages 246-50.
Robert N. Emde, MD, Robert J. Harmon, MD, David Metcalf, MD, Kenneth L. Koenig, MD and Samuel Wagonfeld, MD, "Stress and Neonatal Sleep" PSYCHOSOMATIC MEDICINE, Vol 33, No. 6 (November-December 1971)
Pages 491-497.
Cynthia R. Howard, MD; Fred M. Howard, MD; and Michael L. Weitzman, MD, "ACETAMINOPHEN ANALGESIA IN NEONATAL CIRCUMCISION: THE EFFECT ON PAIN", PEDIATRICS, Volume 93 Nunber 4: Pages 641-646. April 1994.
Marshall RE, Stratton WC, Moore JA, et al. "Circumcision I: effects upon newborn behavior" Infant Behavior and Devopment 1980;3:1-14.
Marshall RE, Porter FL, Rogers AG, et al. "Circumcision: II: effects upon mother-infant interaction" Early Hum Dev 1982; 7:367-374.
Pisacane A, Graziano L. Mazzarella G. Breast-feeding and urinary tract
infection. J Pediatr. 1992;120:87-89.
9. Wiswell TE. Circumcision: an update. Curr Probl Pediatr. 1992;22:424-431
10. Dixon S, Snyder J, Holve R, Bromberger P. Behavioral effects of circumcision with and without anesthesia. J Dev Behav Pediatr. 1984;5246-5250
11. Marshall RE, Porter FL, Rogers AG, Moore J, Anderson B, Boxerman SB. Circumcision II: effects upon mother-infant interaction. Early Hum Dev. 1982;7:367-374
12. Lander J, Brady-Fryer B, Metcalfe JB, Nazarali S, Muttitt S. Comparison of ring block, dorsal penile nerve block, and topical anesthesia for neonatal circumcision: a randomized controlled trial. JAMA. 1997;278:2157-2162
13. Stang HJ, Snellman LW, Condon LM, et al. Beyond dorsal penile nerve block: a more humane circumcision. Pediatrics. 1997;100(2). Available at: URL: http://www.pediatrics.org/cgi/content/full/100/2/e3
14. Blass EM, Hoffmeyer LB. Sucrose as an analgesic for newborn infants. Pediatrics. 1991;87:215-218
15. Taddio A, Stevens B, Craig K, et al. Efficacy and safety of lidocaine-prilocaine cream for pain during circumcision. N Engl J Med. 1997;336:1197-1201
16. Kurtis PS, DeSilva HM, Bernstein BA, et al. A comparison of Mogen and Gomco clamps in combination with dorsal penile nerve block in minimizing the pain of neonatal circumcision. Pediatrics. 1999;103(2). Available at: URL: http://www.pediatrics.org/cgi/content/full/103/2/e23
17. Schoen EJ, Fischell AA. Pain in neonatal circumcision. Clin Pediatr (Phila). 1991;30:429-432
| |




