| |
Ethics of Circumcision
1. Children and
bioethics
Infant circumcision,
instituted without any clinical trials and investigated only after it
was customary, deserves much the same ethical scrutiny as
non-therapeutic research. At present it is held to a much lower ethical
standard - if any.
The following is from the Encyclopedia of
Bioethics, Free Press (Macmillin) London, 1978.
My emphasis in red.
|
CHILDREN AND BIOMEDICINE
Implicit in all deprivations of equal status for
children is the notion that it is permissible for an adult to
substitute his judgment for that of the child (Dworkin; Schrag), based
on the assumptions that the adult has the best interests of the child
at heart, and that he or she is better qualified than the child to make
decisions in the child's interest. While these assumptions are true
enough to gain acceptance as general principles, the exceptions are
sufficiently common to arouse concern (Fost; McCollum and Schwartz;
Robertson and Fost). This
concern over paternalism applies to purely therapeutic as well as
experimental interventions. ... a parent who
initiates a behavior modification program for his child's bed-wetting
may be primarily seeking relief of his own annoyance and might have
difficulty establishing that the benefit-risk ratio of the behavior
program is more advantageous to the child than continuation of the
symptom....
Experimentation in children
The many and complex problems of human
experimentation are compounded in the pediatric setting by four
factors. First, children are not simply small adults, but are
biologically different in many ways, so that knowledge acquired from
adult subjects often cannot be applied to children without testing
them. ... Physical injuries that might be trivial in a mature person
(such as radiation of the growing portion of a long bone [or
damage to the penis - HY]) can become magnified when
occurring early in the developmental process. Events that may have
little psychological significance for an adult, such as a short
hospitalization or repeated venipunctures, may have profound
detrimental effects on a child. Fourth, uncoerced informned consent,
the keystone of protection of human subjects, is often unattainable
from the minor [and never obtainable from the newborn - HY].
There is broad consensus that therapeutic
expenmentation - nonstandard interventions that have the explicit
primary intent of helping the subject to whom they are being applied -
can be practiced in children without major modification of the rules
that apply to experimentation in general, so long as consent from a
legally authorized representative is given (Curran and Beecher; Great
Britain; World Medical Associaton). This is not to imply that the
present regulation of of adult experimentation is satisfactory, or that
parental consent for nontherapeutic experimentation is satisfactory.
But it is in the realm of nontherapeutic experimentation where concerns
are greatest. Ideally, risk, benefit. and consent should all reside in
the same person. When
nontherapeutic research is conducted on a child, it is the child who
bears the risk, while future persons gain the
possible benefits, and a
third party, without risk or benefit, gives consent.
Whether or not parents can legally consent to
nontherapeutic interventions on their children is unresolved. The
Nuremberg Code does not mention children but implies they should be
excluded as subjects by stating it is absolutely essential ... that the
person involved should have legal capacity to give consent." The
Declaration of Helsinki allows nontherapeutic studies on children with
consent of the legal guardian. Current (1976) regulations of the U.S.
Department of Health, Education, and Welfare (DHEW) do not distinguish
between the right of the guardian to consent for nontherapeutic versus
therapeutic research.
...The case of Neilsen v. Regents of
University of California raised, for the first time, the
explicit question of whether a parent may volunteer a child for
nontherapeutic research.
Related cases come from the field of
transplantation, arising when physicians and/or parents seek to use a
legally incompetent person as kidney donor for a relative. The general
response of courts has been to require a finding of benefit for the
donor, such as the advantages derived from future experiences with the
recipient should he survive, or the avoidance of remorse due to loss of
companionship or later guilt from realizing that one had failed to come
to the aid of his sibling (Baron, Botsford, and Cole). In instances
where the donor was incapable of experiencing such benefit because of
severe mental disability or where the social contact with the sibling
was not close, permission to allow the transplantation has been denied (Lausier
v. Pescinski; In re Richardson). While
many of the cases regarding incompetent donors involved intelligent
adolescents or retarded adults, the general principle of the legitimacy
of proxy consent would seem applicable to children in general, and at
least one appellate case did involve a seven-year-old donor (Hart
v. Brown).
In contrast is the famous and much disputed case
of Bonner v. Moran, in which an appellate court
ruled that a skin graft taken from a fifteen-year-old boy could not be
upheld unless the mother consented. One legal scholar takes the
decision to imply that such parental consent would have made the
procedure valid, despite the absence of a direct benefit (Curran and
Beecher), but the decision as written leaves room for disagreement as
to how much it can be extended to nontherapeutic experimentation
(Capron).
In Great Britain the Medical Research Council has
stated that "parents and
guardians of minors cannot give consent on their behalf to any
procedures which are of no particular benefit to them and which may
carry some risk of harm," although legal
precedent or authority for this is obscure (Curran and Beecher).
Proxy consent
As with other ethical issues, the already complex
and unresolved problems of consent are compounded when children are
involved. The assumption that parents can provide uncoerced informed
consent for their children rests at least on the presumption that they
can provide it for themselves. There
is evidence that educated, competent adults are frequently not
adequately informed to give meaningful consent (Fellner
and Marshall; Fletcher; Gray),
so their ability to speak for others may be questioned.
The barriers may not be so much a lack of intelligence or motivation on
the part of patient or physician as more complex forces such as the
anxiety of illness, the intimidating milieu of the hospital, and a
sense of awe, trust, and dependence on the physician-all of which may
conspire to make solicitation of consent a ritual wherein few are
meaningfully informed (Ingelfinger).
In addition to these general barriers to informed
consent, there are aspects peculiar to the parent-child relationship
that complicate the matter further. The perceived vulnerability of the
child may evoke excessive anxiety, which further clouds judgment. The
parent may be acting out unconscious hostile wishes against the child,
particularly if he is retarded or deformed. There may be a wish to
repay the physician-investigator for prior service by offering the
child as a sacrifice.
Even if these obstacles were overcome, the
practice of proxy consent rests on other notions under challenge: the
claim that a person may ever consent to a nontherapeutic intervention
on another (Ramsey, 1970, 1976); the assumption that adults can
reliably assess what is in a child's best interest; and the faith that
they are capable of acting in a person's best interest, even if it can
be accurately identified. The observation that adults frequently cannot
identify or act in their own best interest - as manifested by decisions
ranging from smoking and drinking to marriage and financial investments
- undermines these assumptions.
Two common justifications for proxy consent are
the substituted judgment doctrine, a legal doctrine
which suggests that decisions be based on what the person would be
likely to do if competent (Robertson), and the ethical notion that a
child can be volunteered on the basis of what he ought
to do (McCormick).
The
substituted judgment doctrine is weakened by the inability of an adult
to know the child's mind. Put another way, the
adult may err by being able only to imagine what a reasonable adult
would do if in the situation of the child, thereby fallaciously
equating adult values and preferences with those of children. An adult
might gladly consent to a venepuncture, a procedure of minimal risk and
annoyance, but for a child the same event could be a major
psychological trauma. Presumptions of what adults would do may suffer
from misperceptions of the empirical situation. One could presume that
adults probably would consent to minimally hazardous nontherapeutic
procedures, but in many communities they in fact do not participate,
unless offered significant inducements. One implication of this might
be that a minimum requirement for the use of nonconsenting children in
non therapeutic studies (assuming other objections can be overcome)
would include some age-appropriate indirect benefit or reward
comparable to the monetary rewards that an adult would receive.
McCormick has argued that children may be used for
nontherapeutic studies to which they ought to
consent, on the grounds that there are some sacrifices all members of
the human community ought to make, and it is in their interest to do
so. While there might be agreement on what sacrifices people ought to
make, many would object to the recruitment of children without their
consent, unless adults were also required to participate on the same
grounds, unrelated to their consent.
Ramsey has taken the extreme view that proxy
consent for nonbeneficial experiments in children are unethical without
qualification (Ramsey, 1970). He later modified this by acknowledging
that such research might be done so long as one acknowledged that he
was "doing wrong for the sake of the public good" (1976). Reluctantly
admitting that it might be wrong, in some circumstances, not
to do the research, he seemed to be pointing up an aspect of all true
ethical dilemmas: that they involve conflicts of two important
obligations, with the inevitable consequence that something of value
will be lost no matter which way the conflict is resolved.
As the child gets older - and intellectual and
emotional maturity allow him increasingly to participate in decisions -
some have advocated a requirement that the child consent in addition to
the parent, even though the child may be legally incompetent (U.S.
DHFW, National Institutes of Health). While such a practice sounds
appealing, there is some evidence that a principle may be honored at
the expense of the child's emotional well-being. One study concluded
that children informed of the research nature of their hospitalization
experienced overwhelming anxiety, due in part to fantasies aroused by
their primitive notions of research (Schwartz).
Rules based on inflexible age boundaries may not
serve the needs of individual persons. Many children can and should be
included in discussions of their participation in research; many adults
are incapable of participating meaningfully. Ideally, decisions would
be based on a full consideration of the facts in each case, including
the probability of discomfort and risk and the emotional and
intellectual capacity for consent in each child.
Requirements
for consent serve two functions: protection from unacceptable risks and
respect for the autonomy of each individual. It
appears that trust in consent as protection from unacceptable risks has
been misplaced (Fletcher; Gray) and, in the case of young children,
respecting autonomy may be impossible unless nontherapeutic research is
avoided entirely. If such studies are to continue, it will be necessary
to pay attention to Ramsey's reminder that it
is not an unmitigated good, that something of value is being lost, and
that it is possible for a subject to be "wronged without being harmed"
(Ramsey, 1970).
|
2. A more direct approach
A Canadian ethicist, Dr Margaret Somerville (Gale
professor of law and a professor in the faculty of medicine at the
McGill Centre for Medicine, Ethics and Law), has addressed the issue of
infant male circumcision directly. Here are excerpts from an article
she wrote (in The Gazette, Montreal, on October 24, 1998, pB6):
|
"The usual ethical and legal justification of any
parent-sanctioned surgical wounding of a child is that this must be
undertaken with a therapeutic intent.
"As the Canadian Pediatric Society has recognized,
routine infant male circumcision is not therapeutically necessary.
Parents cannot give an informed consent to non-therapeutic
interventions on their children that involve any more than the most
trivial harm. Infant male circumcision does not fall within this
description,...
"I believe that it does [have harmful effects],
including the irreversible loss of healthy, erogenous tissue, the risks
involved in the procedure itself and the pain that this procedure
involves.
"We need to keep in mind an old saying in human
rights: "Nowhere are human rights more threatened than when we act
purporting to do good". This is true because when we are seeking to do
good, we can be insensitive to the fact that our conduct also involves
doing harm.
"Respect for [children's human] rights requires
that we must have very substantial justification for subjecting a child
to any risk through a surgical intervention, causing him pain or
intervening to alter his body permanently, other than to provide
necessary therapy for the child himself."
|
(Somerville's article was in answer to an HIV researcher
who was defending circumcision to prevent HIV. Some other excerpts from
this article are included on the page about HIV.)
Somerville has now written a book about ethics
including a chapter about infant
circumcision.
3. The American
Medical Association's Principles of Ethics
The AMA has revised its Principles of Medical Ethics to
add parts VIII and
IX. The revised Principles were adopted in June 2001 by the AMA House
of
Delegates.
E- Principles of Medical
Ethics
Preamble:
The medical profession has long subscribed to a body of
ethical statements
developed primarily for the benefit of the patient. As a member of this
profession, a physician must recognize responsibility
to patients first
and foremost, as well as to society, to other health
professionals, and to
self. The following Principles adopted by the American Medical
Association
are not laws, but standards of conduct which define the essentials of
honorable behavior for the physician.
I. A physician shall be dedicated to providing competent
medical care,
with compassion and respect for human dignity and
rights.
II. A physician shall uphold the standards of
professionalism, be honest
in all professional interactions, and strive to report physicians
deficient in character or competence, or engaging in fraud or
deception,
to appropriate entities.
III. A physician shall respect the law and also
recognize a responsibility
to seek changes in those requirements which are contrary to the best
interests of the patient.
IV. A physician shall respect
the rights of patients, colleagues, and
other health professionals, and shall safeguard patient confidences and
privacy within the constraints of the law.
V. A physician shall continue to study, apply, and
advance scientific
knowledge, maintain a commitment to medical education, make relevant
information available to patients, colleagues, and the public, obtain
consultation, and use the talents of other health professionals when
indicated.
VI. A physician shall, in the provision of appropriate
patient care,
except in emergencies, be free to choose whom to serve, with whom to
associate, and the environment in which to provide medical care.
VII. A physician shall recognize a responsibility to
participate in
activities contributing to the improvement of the community and the
betterment of public health.
VIII. A physician shall, while caring for a patient,
regard responsibility to the patient
as paramount. [...and not
to his parents or caregivers.]
IX. A physician shall support access to medical care for
all people.
The AMA's Council on Scientific Affairs (not its Council
on Ethical and Judicial Affairs) has prepared a policy
statement on neonatal circumcision that makes no reference to
these concerns.
3a. the American
Medical Association Code of Ethics
|
3.6
Regardless of society's attitudes, do not
countenance, condone or participate in the practice of torture or other
forms of cruel, inhuman, or degrading procedures, whatever the offence
of which the victim of such procedures is suspected, accused or
convicted.
|
[4. Ban called for
in Sweden This item has been moved to the page on events in Sweden.]
5. The Ethical
Triangle
As the Encyclopedia
of Bioethics item points out, there are three parties
involved in a circumcision (four if the parents disagree). Their power
and information relationships are wildly unequal:
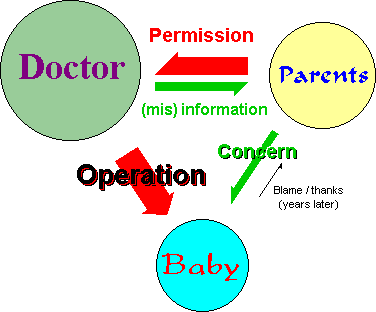
While the baby has no power, he experiences virtually
all of the effects of the circumcision. For this reason, it is
ethically lacking for the AAP
and the AMA to say the
parents should decide, based on whatever information they may have.
If the parents disagree, the present position in the US
is that either may give permission for him to be circumcised. In the
UK, both must. For an elective procedure now agreed by the AMA to be
"non-therapeutic", the US position is untenable.
6. Petition
You can endorse the
Ashley Montagu Resolution to End the Genital Mutilation of Children
Worldwide, a Petition to the World Court, the Hague
(offsite).
7. An extract from
a textbook of medical ethics
Parental
decisions regarding treatment options
In most jusrisdictions there is a fuzzy boundary between
the age at which a child can give consent to her own treatment and the
age at which parental consent must be sought. Most ethicists advise
that the child be included as far as possible in the decision-making
process, but for childre up to at least 16 years old, the parents
should give consent to medical treatment.
The basis for the parental right to to choose treatment
for children rests in the intuition that parents are protectors of the
child and responsible for the child's care. This is regarded as the
'natural role' of parents and is recognised universally in legal codes.
It is assumed that the parent is training and nurturing the child to
bring that child to the point where she can make her own decisions. We
act on the presumption that the parents will make decisions in the best
interests of the child and, on this basis, empower them to do so.
However, in certain situations, this presumption cannot be sustained.
[example of parents withholding blood transfusion on
religious grounds] ... the child is made a ward of the court for the
the duration of her treatment because the court believes that the
parents are not acting in the best interest of the child.
This decision shows what we believe to be paramount in
dilemmas involving children. We
believe that the child's interests should come first.
Alastair Campbell, Grant Gillett
and Gareth Jones
"Practical Medical Ethics" Oxford University Press
Auckland, 1992, p75
8. A
faulty article
9. "Dual loyalty"
and conflict of interest
|
The Problem of Dual Loyalty and
Human Rights for Physicians
The organization Physicians for Human Rights has a
publication authored
by dozens of doctors around the globe on "The Problem of Dual Loyalty
and
Human Rights" in regards to physicians.
From the introduction:
The problem of dual loyalty - simultaneous
obligations, express or
implied, to a patient and to a third party, often the state - continues
to challenge
health professionals. Health professional ethics have long stressed the
need
for loyalty to people in their care. In the modern world, however,
health
professionals are increasingly asked to weigh their devotion to
patients
against service to the objectives of government or other third parties.
Dual
loyalty poses particular challenges for health professionals throughout
the world
when the subordination of the patient's interests to state or other
purposes
risks violating the patient's human rights.
Since ancient times, many societies have held
healthcare professionals to
an ethic of undivided loyalty to the welfare of the patient. Current
international codes of ethics generally mandate complete loyalty to
patients. The
World Medical Association (WMA) Declaration of Geneva, the modern
equivalent of the Hippocratic Oath, asks physicians to pledge that "the
health of my patient
shall be my first consideration" and to provide medical services in
"full
technical and moral independence." The WMA International Code of
Medical Ethics states that "a physician shall owe his patients complete
loyalty and all the
resources of his science."
In practice, however, health professionals often
have obligations to
other parties besides their patients - such as family members,
employers,
insurance companies and governments - that may conflict with undivided
devotion to the patient. This phenomenon is dual loyalty, which may be
defined as clinical
role conflict between professional duties to a patient and obligations,
express
or implied, real or perceived, to the interests of a third party such
as an
employer, an insurer or the state. The dual loyalty problem is usually
understood in the context of a relationship with an individual patient.
In
many parts of the world, however, clinicians have responsibilities to
communities of patients, for prevention, health education and clinical
care. Dual
loyalty conflicts can and do arise in these settings as well.
The
article in full
|
10. An important article.
|
JOURNAL
OF MEDICAL ETHICS (U.K.), Vol 30: Pages 248-253,
June 2004.
SYMPOSIUM ON CIRCUMCISION
Rationalising
circumcision: from tradition to fashion, from public health to
individual freedom-critical notes on cultural persistence of the
practice of genital mutilation
S K Hellsten
(Abstract:) Despite global and local attempts to
end genital mutilation, in their various forms, whether of males or
females, the practice has persisted throughout human history in most
parts of the world. Various medical, scientific, hygienic, aesthetic,
religious, and cultural reasons have been used to justify it. In this
symposium on circumcision, against the background of the other articles
by Hutson, Short, and Viens, the practice is set by the author within a
wider, global context by discussing a range of rationalisations used to
support different types of genital mutilation throughout time and
across the globe. It is argued that in most cases the rationalisations
invented to provide support for continuing the practice of genital
mutilation-whether male or female-within various cultural and religious
settings have very little to do with finding a critical and reflective
moral justification for these practices. In order to question the
ethical acceptability of the practice in its non-therapeutic forms, we
need to focus on child rights protection.
|
This is one of the first articles in an ethical journal
seriously to criticise routine (non-medically indicated) infant
circumcision side by side with FGM from an ethical perspective. It
carefully considers individual vs collective rights and comes firmly
down on the right of the child to bodily integrity and autonomy.
11. AMA Council on
Ethical and Judicial Affairs
|
Here are some opinions from the
AMA Council on Ethical and Judicial
Affairs that are relevant to the practice of circumcision.
E-2.035 Futile Care
Physicians are not ethically obligated to deliver care that, in their
best
professional judgment, will not have a reasonable chance of benefiting
their patients. Patients should not be given treatments simply because
they demand them. Denial of treatment should be justified by reliance
on
openly stated ethical principles and acceptable standards of care, as
defined in Opinion 2.03, "Allocation of Limited Medical Resources," and
Opinion 2.095, "The Provision of Adequate Health Care," not on the
concept
of "futility," which cannot be meaningfully defined.
(I, IV) Issued June
1994.
E-3.01 Nonscientific Practitioners
It is unethical to engage in or to aid and abet in treatment which has
no
scientific basis and is dangerous, is calculated to deceive the patient
by
giving false hope, or which may cause the patient to delay in seeking
proper care. Physicians should also be mindful of state laws which
prohibit a physician from aiding and abetting an unlicensed person in
the
practice of medicine, aiding or abetting a person with a limited
license
in providing services beyond the scope of his or her license, or
undertaking the joint medical treatment of patients under the foregoing
circumstances. Physicians are otherwise free to accept or decline to
serve
anyone who seeks their services, regardless of who has recommended that
the individual see the physician.
(III, VI) Issued prior to April 1977;
Updated June 1994 and June 1996.
E-8.20 Invalid Medical Treatment
The following general guidelines are offered to serve physicians when
they
are called upon to decide among treatments:
(1) Treatments which have no medical indication and offer no possible
benefit to the patient should not
be used (Opinion 2.035, "Futile Care").
(2) Treatments which have been
determined scientifically to be invalid should not be used (Opinion
3.01,
"Nonscientific Practitioners").
(3) Among the treatments that are
scientifically valid, medically indicated, and offer a reasonable
chance
of benefit for patients, some are regulated or prohibited by law;
physicians should comply with these laws. If physicians disagree with
such
laws, they should seek to change them.
(4) Among the various treatments
that are scientifically valid, medically indicated, legal, and offer a
reasonable chance of benefit for patients, the decision of which
treatment
to use should be made between the physician and patient.
(I, III, IV)
Issued June 1998 based on the report "Invalid Medical Treatment,"
adopted
December 1997.
E-10.05 Potential Patients
(1) Physicians must keep their professional obligations to provide care
to
patients in accord with their prerogative to choose whether to enter
into
a patient-physician relationship.
(2) The following instances identify the
limits on physicians' prerogative:
(a) Physicians should respond to the
best of their ability in cases of medical emergency (Opinion 8.11,
"Neglect of Patient").
(b) Physicians cannot refuse to care for patients
based on race, gender, sexual orientation, or any other criteria that
would constitute invidious discrimination (Opinion 9.12,
"Patient-Physician Relationship: Respect for Law and Human Rights"),
nor
can they discriminate against patients with infectious diseases
(Opinion
2.23, "HIV Testing").
(c) Physicians may not refuse to care for patients
when operating under a contractual arrangement that requires them to
treat
(Opinion 10.015, "The Patient-Physician Relationship"). Exceptions to
this
requirement may exist when patient care is ultimately compromised by
the
contractual arrangement.
(3) In situations not covered above, it may be
ethically permissible for physicians to decline a potential patient
when:
(a) The treatment request is beyond the physician's current competence.
(b) The treatment request is known to be scientifically invalid, has no
medical indication, and offers no possible benefit to the patient
(Opinion
8.20, "Invalid Medical Treatment").
(c) A specific treatment sought by an
individual is incompatible with the physician's personal, religious, or
moral beliefs.
(4) Physicians, as professionals and members of society,
should work to assure access to adequate health care (Opinion 10.01,
"Fundamental Elements of the Patient-Physician Relationship").*
Accordingly, physicians have an obligation to share in providing
charity
care (Opinion 9.065, "Caring for the Poor") but not to the degree that
would seriously compromise the care provided to existing patients. When
deciding whether to take on a new patient, physicians should consider
the
individual's need for medical service along with the needs of their
current patients. Greater medical necessity of a service engenders a
stronger obligation to treat.
(I, VI, VIII, IX) Issued December 2000 based
on the report "Potential Patients, Ethical Considerations," adopted
June
2000. Updated December 2003.
* Considerations in determining an adequate
level of health care are outlined in Opinion 2.095, "The Provision of
Adequate Health Care."
|
12. New study finds
circumcision unethical
|
LAW, ETHICS, AND MEDICINE
A covenant with the status quo? Male circumcision
and the new BMA guidance
to doctors
M Fox and M Thomson
School of Law, Keele University, Staffordshire, UK
ABSTRACT
This article offers a critique of the recently revised BMA guidance on
routine neonatal male circumcision and seeks to challenge the
assumptions
underpinning the guidance which construe this procedure as a matter of
parental choice. Our aim is to problematise continued professional
willingness to tolerate the non-therapeutic, non-consensual excision of
healthy tissue, arguing that in this context both professional guidance
and law are uncharacteristically tolerant of risks inflicted on young
children, given the absence of clear medical benefits. By interrogating
historical medical explanations for this practice, which continue to
surface in contemporary justifications of non-consensual male
circumcision, we demonstrate how circumcision has long existed as a
procedure in need of a justification. We conclude that it is ethically
inappropriate to subject children-male or female-to the acknowledged
risks
of circumcision and contend that there is no compelling legal authority
for the common view that male circumcision is lawful.
Full text: Journal
of Medical Ethics 2005;31:463-469
If this link breaks, email me.
|
14. Doctor admits
existing consent form understates risks.
|
From
the PSOT blog
To Plastibell
or Not To Plastibell?
Comment for the STFM procedure list dialog on
Circumcison Techniques.
I have been unhappy with the Plastibell device...
Mogen is the easiest and fastest with excellent
safety, but lack of fundamental skills with needle and thread
intimidate many from being able to do these procedures past the newborn
period.
Since we started Medicos, we have stopped doing
circumcisions in the hospital. Our group concensus is that these are cosmetic procedures
performed due to cultural influences within the family. We encourage family to consider them
carefully and weigh the decision carefully. The immediate
newborn period is a complex one in an artificial environment. We do circumcisions at the
first visit which ranges from 2d to 2 months. I will perform Gomcos and
Mogens up to 2 years of age with the occasional need to use sutures for
bleeders.
Wm MacMillan Rodney MD
Adjunct Professor of Family Medicine
Adjunct Professor Surgery/Emergency Medicine
Meharry/Vanderbilt School of Medicine
Medicos para la Familia
Memphis and Nashville, Tn.
www.psot.com
REPLY from PFENNINGER 2 years? How do you tie the little tykes down? Do you
sedate them? After about 2 months they are too big for the
papoose board. I too do them in the office if they aren�t done in the
nursery. Gomco. Hospital wants $700 to do in day surgery!!! So, I just
bought the instruments and board for the office. As they get older, I
find it harder to do�.to keep them from squirming all over.JP
REPLY-WMR Haven't you gotten a copy my book on
health care for the Uninsured? In addition, Rodney's Manual of Redneck
Medicine suggests that children can
be successfully restrained using John Deere blankets and an assistant
named Bubba.
[We
think he is being satirical, but the reality is unlikely to be much
different.]
...REPLY -WMR I've never seen a long term
complication from a Gomco, but continue to believe that the procedure is not medically indicated.
.
... REPLY WMR--Every
50 or so I intentionally use some vicryl suture as a "teachable moment".
I choose Vicryl because it is soft and I believe its ends are less
traumatic than gut which is bristly. Every once and awhile I will do some free hand circ technique[DR.
90210] under the guise of making a more beautiful penis.
These moments are used to demonstrate common hemostatic techniques with
suture material can apply to this procedure as easily as to perineal
repair.
[In
other words he uses babies as teaching aids, falsifying his action to
the parents. The arrogance of claiming to "make" a penis more beautiful
by surgery defies belief.]
As family physicians I would be willing to lead a
study giving informed consent to parents [I'll show you mine at 2 days
if you'll show me yours at 2 days], and ask the average parent to
choose which technique they would prefer. If we did a true informed consent about the
medical benefits versus risks, they would probably choose neither.
However using the standard consent, I imagine there would be a
statistically significant preference for the nonPlastibell methods
Wm MacMillan Rodney MD
Adjunct Professor of Family Medicine
Meharry/Vanderbilt School of Medicine
Medicos para la Familia
Memphis and Nashville, Tn.
www.psot.com
See also complications
for more admissions from this doctor.
|
15. Norwegian Medical
Association finds ritual circumcision unethical
|
Journal
of the Norwegian Medical Association, Volume 121
Number 25: Page 2994, 20 October 2001
Ritual
Circumcision of Boys
The Council for
Medical Ethics states that ritual circumcision of boys is
not consistent with important principles of medical ethics, that it is
without medical value, and should not be paid for with public funds.
The council has sent a
statement to the board of the Norwegian Medical
Association on this matter. Among other things, the council says that
ritual circumcision of boys has no established medical benefit. Even
with
the use of local anaesthesia, the procedure causes pain and is
associated
with certain risks of medical complications. The Council for Medical
Ethics states that circumcision of boys is not consistent with
important
principles of medical ethics laid down as general determinations in
Paragraph 1 (� 1) of the Norwegian Code of Ethics for Doctors. These
require doctors to uphold human health, and to cure, relieve and
comfort.
The council points out that it is an important factor that the child
cannot give consent.
According to the
council, doctors should be allowed to refuse to perform
ritual circumcision as a matter of conscience. The council makes a
point
of noting that, when performed, even if not for medical reasons, that
circumcision is a surgical operation that must be carried out according
to
correct principles of surgery and with proper anaesthesia. In line with
the Code of Ethics for Doctors � 12, it should not be paid for by the
public health service.
The council invited
relevant religious leaders in our community to work on
replacing circumcision with symbolic rituals that do not involve a
surgical procedure.
P�l Gulbrandsen
|
Tidsskrift for den Norske laegeforening
2001; 121: 2994 utga
Rituell
omskj�ring av gutter
R�det for legeetikk mener at rituell omskj�ring av
gutter ikke er i tr�d med viktige legeetiske prinsipper, at det er uten
medisinsk nytteverdi og ikke b�r bekostes av det offentlige.
R�det har sendt en uttalelse til sentralstyret i
Legeforeningen i sakens anledning. Der heter det bl.a. at rituell
omskj�ring av gutter ikke har etablert medisinsk nytteverdi. Selv ved
bruk av lokalbed�velse medf�rer inngrepet smerte og er forbundet med en
viss risiko for medisinske komplikasjoner. R�det for legeetikk mener at
omskj�ring av guttebarn ikke er i tr�d med viktige legeetiske
prinsipper nedfelt i de alminnelige bestemmelsene i � 1 i Etiske regler
for leger. Disse p�legger leger � verne menneskets helse, og �
helbrede, lindre og tr�ste. R�det p�peker at det er et viktig moment at
barn ikke kan gi samtykke.
If�lge r�det m� leger ogs� kunne reservere seg mot � foreta rituell
omskj�ring av samvittighetsgrunner. Selv om inngrepet ikke utf�res p�
medisinsk indikasjon, p�pekes det likevel at omskj�ring er et kirurgisk
inngrep som bare m� utf�res etter anerkjente kirurgiske prinsipper og
med optimal bed�velse. I tr�d med Etiske regler for leger � 12 b�r det
ikke kreves at utgiftene belastes det offentlige helsevesen.
R�det oppfordrer aktuelle religi�se ledere i v�rt samfunn om � arbeide
for � erstatte omskj�ring med symbolske ritualer som ikke inneb�rer et
kirurgisk inngrep.
Ref: Tidsskr Nor L�geforen 2001; 121: 2994 utga
pal.gulbrandsen@legeforeningen.no
|
17. Dr Jeykell and Mr Hyde
| It
is hard to believe the same person was involved in writing these two
papers, just 14 months apart. Both speak with the authority you'd
expect from a Jesuit Professor of Ethics, but the first is more
carefully argued, more nuanced and has 64 references, compared to the
second with only 25 (of which the first paper is one). The first makes
extensive references to previous Catholic teaching, the second, none.
Theories about why Prof. Clark did this include demonic possession, but
more likely is that he meant to mark his student's essay F, but then
accidentally put it in the wrong envelope. |
Health
Progress
September-October 2006 Volume 87, Number 5
To Circumcise or Not to Circumcise?
A Catholic Ethicist Argues That the
Practice Is Not in the Best Interest of
Male Infants
BY FR. PETER A. CLARK, SJ, PhD
Fr. Clark is professor, theology and health administration, and
director,
Institute of Catholic Bioethics, Saint Joseph's University; as well as
bioethicist, Mercy Health System. Both organizations are in
Philadelphia.
Routine neonatal male circumcision is the most
frequent surgical operation
performed on males in the United States. In recent years, however,
there
has been a widespread debate in the medical, ethical and, most
recently,
the legal communities concerning the surgery's appropriateness. At
first
glance, the issue appears to be solely medical. But, after further
analysis, one can see that it has religious, cultural, and even
socioeconomic implications. A comprehensive review of the medical
literature reveals arguments both for and against this routine
procedure.
One writer notes that "of the at least 16 national and international
medical organizations that have spoken on routine neonatal
circumcision,
not a single group has recommended it. This includes five leading
American
organizations, including the American Medical Association and the
American
Academy of Pediatrics."
...
Neonatal male circumcision fails the test of
beneficence because the minor
benefits that might result from the procedure do not outweigh its
potential
harms and risks. Indeed, recent policy statements issued by
professional
societies representing Australian, Canadian, and American pediatricians
do
not recommend routine circumcision. The procedure also fails the test
of
nonmaleficence because the removal of functioning, healthy body tissue
in
the name of tradition, custom, or a non-disease-related cause
intentionally
inflicts bodily harm, injury, and, in rare cases, even death on
vulnerable
minors. This is clearly contrary to the basic tenet of medical ethics:
"First do no harm."
Justice
This principle recognizes that each person should
be treated fairly and
equitably and be given his or her due. It can be applied to neonatal
circumcision in two ways.
First, questions of justice have been raised about
the legal right to
bodily integrity of these vulnerable patients. One problem with
circumcision, besides pain and possible complications, is the loss by
the
infant of the inherent value of an intact penis. To circumcise a person
is
to violate his bodily integrity, which is a direct violation of the
principle of justice. Many people see male circumcision as cruel and
degrading because it detracts from the appearance and function of the
male
sex organ by removing large amounts of healthy, functional, protective
erogenous tissue. To mutilate and degrade any individual is a violation
of
the principle of justice.
Second, circumcision specifically involves the
issue of distributive
justice, which concerns the fair and equitable allocation of medical
resources. As noted, more than a million U.S. males are circumcised
each
year, at a cost estimated to be as high as $270 million. A cost-benefit
analysis of neonatal male circumcision has found it not to be cost
effective; indeed, in contrast to most medical interventions, which
cost
money but preserve or restore health, neonatal male circumcision costs
money and may reduce health. Today the United States has 46 million
uninsured people and countless others who are underinsured. Spending
hundreds of millions of dollars a year on a nontherapeutic surgery that
has, at best, debatable benefits for the child is a direct violation of
the
principle of distributive justice. The primary beneficiary of male
circumcision seems to be the medical community. As an organization
opposed
to the procedure notes, "Physicians receive an estimated $200 million
in
fees for 1,100,000 circumcisions performed annually in the United
States,
while hospitals receive an estimated $500 million due to longer stays
for
both mother and infant when circumcision is performed."
Medical resources in this country and worldwide are limited and must be
conserved. Proper stewardship of these resources entails not wasting
them
on treatments that have questionable outcomes and can be deemed
inappropriate. These resources must be rationally allocated; to waste
them
is ethically irresponsible and morally objectionable.
The Catholic Perspective
In the Ethical and Religious Directives for
Catholic Health Care Services
(ERDs), Directive 29 states clearly that "bodily integrity" must always
be
respected:
"All persons served by Catholic health care have
the right and duty to
protect and preserve their bodily and functional integrity. The
functional
integrity of the person may be sacrificed to maintain the health or
life of
the person when no other morally permissible means is available."
Directive 33 states that any therapeutic procedure
that causes harm to apatient can be justified
only if the benefits outweigh the burdens: "The well-being of the whole
person must be taken into
account in deciding about any therapeutic intervention or use of
technology. Therapeutic procedures
that are likely to cause harm or undesirable side-effects can be
justified only by a proportionate
benefit to the patient." The Catechism of the Catholic Church states
that "except when performed
for strictly therapeutic reasons, directly intended amputations,
mutilations, and sterilizations
performed on innocent persons are against the moral law." Examining
neonatal male circumcision in
light of these moral directives, one can conclude that the amputation
of normal, healthy foreskin
for nontherapeutic purposes not only violates the child;s bodily
integrity but also is a medical
procedure whose benefits do not clearly outweigh the risks.
...
The Catholic Church teaches that God created us in God;s image and
likeness (Gn 1:27-28).
It follows then that God created males with normal, healthy foreskins
for the purpose of protecting
the glans, providing natural lubrication to prevent dryness, and
contributing significantly to the
sexual response of the intact male. To surgically remove the foreskin
for hygienic reasons, and/or
to obtain other questionable benefits that absorb medical resources
costing over $200 million a year
is not only ethically unjustifiable but morally irresponsible,
especially when such procedures can
lead to serious injury and even death. Besides the possible harm the
procedure can inflict on a
child - which violates the basic tenet of Catholic health care of
treating every person with dignity
and respect - it also violates Catholic health care;s mandate to be
responsible stewards of medical
resources. When millions of people in the United States and around the
world lack basic health care,
the provision of a nontherapeutic procedure - especially one that is
unnecessary, costly, and in
some cases fatal - is irresponsible and a violation of the moral law.
...
As the Benatars have noted, "It
is all too easy (and common) to privilege those cultural ways to which
one is accustomed on account
of their familiarity. There is value in stepping back from one;s
cultural assumptions. When one
views male circumcision from another cultural perspective, one can only
wonder what possessed
ancient people to first think of removing the foreskin." To justify
male circumcision for cultural
reasons could be seen as a precedent that supports the justification of
female circumcision for
cultural reasons. To justify one of these practices because of its
cultural acceptance is to start
down the slippery slope toward justifying the other as socially
acceptable. Barring religious
obligation, there is little to recommend routine neonatal male
circumcision. If promoting the
dignity and respect of every human person is a priority for the United
States and for Catholic
health care, then it is time to better educate the public about this
issue and protect those who are
the most vulnerable in our society. Doing so is not only a social
responsibility; it is a moral
imperative as well.
...
|
Med
Sci Monit
December 1, 2007; 13(12): RA205-213
Mandatory[*]
neonatal male circumcision in Sub-Saharan Africa: Medical and ethical
analysis
[* The
term "mandatory is used 30 times in the paper, but nowhere defined.
Whose mandate? The Church? The government? Is the decision whether to
circumcise to be taken away even from the parents?]
Peter A Clark, Justin Eisenman, and Stephen Szapor,
Institute of Catholic Bioethics, St. Joseph's University, Philadelphia,
PA, U.S.A.
[Abstract]
...
Three recent randomized controlled trials undertaken in Kisumu, Kenya,
Raki District, Uganda and Orange Farm, South Africa have confirmed that
male circumcision reduces the risk of heterosexually acquired HIV
infection in men by approximately 51% to 60%. These three studies
provide a solid evidence-base for future health policy. The procedure
for adolescents and adults is expensive compared to abstinence [Anything is expensive compared to
abstinence], condoms [Yet
governments are throwing money at adult circumcision while refusing to
pay for condoms; the authors of this study, of course, have an
ideological objection to the use of condoms at all]
or other methods; and the surgery is not without serious risks if
performed by traditional healers using unsterilized blades as often
happens in rural Africa [It's
not without serious risks if performed by doctors in surgeries, either.].
However, neonatally, the procedure is relatively inexpensive [It is? It demands no less skill,
and requires as much or more equipment] and the
risks diminish considerably [And
the evidence for that is...? The baby's penis is smaller, and any
mistakes on it are magnified when he grows up.].
Mandating neonatal male circumcision is an effective therapy that has
minimal risks, is cost efficient and will save human lives. To deny
individuals access [Strapping
a baby down and cutting part of his penis off is not "giving him access"]
to this effective therapy [whatever
else it is, it's not "therapy"] is to deny them
the dignity and respect all persons deserve. Neonatal male circumcision
is medically necessary and ethically imperative.
From the article:
An uncircumcised penis consists of a
cylindrical shaft and a rounded tip (glans) which is separated
by a tissue groove called the coronal sulcus. [They've
defined the foreskin out of existence, leaving nothing to remove!
(Perhaps they've never seen one...) ] During
the circumcision procedure the foreskin is removed to a point
near the coronal sulcus 8
8. Clark P: To
Circumcise or Not to Circumcise. Health Progress, 2006;
87: 30�39 [The
article on the left, which quotes the AAP definition of the foreskin
and circumcision. The fact that that article diametrically opposes this
one is not acknowledged.]
... The principle
of double effect specifies four conditions that must be
fulfilled for an action with both a good and a bad effect to
be morally justified.
- The action, considered by itself and
independently of its
effects, must not be morally evil. The object of the action
must be good or indifferent.
- The evil effect must not be the means of
producing the
good effect.
- The evil effect is sincerely not intended, but
merely tolerated.
- There must be a proportionate reason for
performing the
action, in spite of its evil consequence.
It should be noted that a number of ethicists known as proportionalists
have argued that the first three conditions of
the principle of double effect are incidental to the principle,
and that in reality it is reducible to the fourth condition
of proportionate reason. While this is a legitimate argument,
it is not the purpose of this article to reopen the
controversy on the validity of the first three conditions. This
article will remain within the framework of the four conditions
of the principle of double effect and apply these
conditions to mandatory neonatal male circumcision as
an effective method of prevention against HIV infection in
sub-Saharan Africa.
The principle of double effect is applicable to
the issue
of mandatory neonatal male circumcision in sub-Saharan
Africa because it has two effects: one good and the other
evil. The good effect is that three recent randomized clinical
trials in Africa have shown that male circumcision reduces the risk of
heterosexually acquired HIV infection in
men by approximately 51% to 60%. The evil effect concerns
the removal of a child�s healthy foreskin without his
informed consent which violates the principle of autonomy.
It also violates the principle of nonmaleficence in that
less invasive and more effective methods of HIV prevention
may be discovered before the child reaches sexual maturity. [They seem to say this and then
forget it.]
Mandatory neonatal male circumcision in sub-Saharan
Africa is ethically justified because it meets the four conditions
of the principle of double effect. [They
assert this, but go nowhere near demonstrating it. This argument is so
simplistic, as if good and evil can be turned on and off like a light
switch, and balanced against each other like apples, it is hard to
believe a Professer of Ethics could have anything to do with writing it.]
... The first condition allows for neonatal male
circumcision
because the action in and of itself is good, in that clinical
research studies have proven that it can effectively reduce
male heterosexual HIV infection by 60%. [Fr
Clark seems to have forgotten what he wrote just 14 months ago.]
... In addition,
male circumcision at a later age can cause more serious
medical complications and is more costly. The medical
complications include pain, hematoma, bleeding, damage
to the penis, infection and even death. [...
exactly as they do at an earlier age.]
... If the guidelines proposed
are implemented and safeguards are assured, then
mandatory neonatal male circumcision is not only medically
necessary, it is ethically imperative. [The
authors give no indication whether or how those conditions can be
fulfilled.] If the protection
and preservation of human life is a priority in sub-Saharan
Africa, then it is time to initiate mandatory neonatal male
circumcision before it is too late for the most vulnerable. [The authors nowhere address the
point made in Fr Clark's earlier article, that we have more than 10
years before childen born today become sexually active.]
This must become an immediate priority, because human
lives hang in the balance.
...
Neonatal circumcision is neither
medically necessary nor ethically permissible: A response to Clark et
al. by Robert S. Van Howe and J. Steven Svoboda will be
published in Med Sci 2008 Aug; 14(8):LE7-13.
|
20. Letter to the British Medical Journal
|
British
Medical Journal
February 19, 2011
Circumcision in boys and girls: why the double
standard?
Personal View
by Mihail Evans
New legislation in France has led to more debate
on whether wearing the veil amounts to the sexual repression of Muslim
women. Islam's treatment of women is a regular topic in the Western
press, yet few jump to the defence of Muslim and other little boys
subjected to childhood circumcision. Indeed, the circumcision of the
grandson of President Sarkozy, ironically a proponent of the veil ban,
made only the gossip pages in France. As a permanent surgical genital
alteration, circumcision is arguably a much more serious matter. After
all, a Muslim woman has, at least in theory, the option to throw away
her veil. The circumcised man's foreskin has been thrown away already.
Few countries have banned male circumcision, but
even symbolic alternatives to female genital mutilation are banned in
almost all Western jurisdictions. While I was a student, a female
academic at my institution published a piece supportive of male
circumcision. This prompted a thought experiment: suppose we found a
male academic supportive of the surgical modification of female
genitals. Would his views be accepted? Why can a Jewish woman speak
openly to defend male circumcision and a Somali man not defend female
circumcision?
Physiological research has undermined beliefs that
the foreskin is "just a flap of skin" and shown it to be an integral
part of the penis. With the foreskin considered an erogenous,
multifunctional tissue, the established view of circumcision as a
non-damaging excision is fatally undermined. It would be more
appropriate to change our terminology, to speak of male genital
mutilation rather than circumcision in the same way that we use female
genital mutilation and not cliteradectomy.
Finland is among the few places where male
circumcision is illegal, although recent judicial decisions have
backtracked on this law, making exceptions for some religious
circumcisions. Bulgaria banned male circumcision in the 1980s, but more
as part of a cultural war on its Muslim minority than out of any
overtly humanitarian concern. My partner is Bulgarian, and it amazes me
that under law in the United Kingdom I could legally take my son there
and subject him to the sort of horrific circumcision recorded by a
Bulgarian current affairs programme (www.vbox7.com/play:72a1576e), yet
my Somali neighbours would be prosecuted for attempting to appease
traditional opinion by replacing female circumcision with a symbolic
pinprick to the clitoral hood.
We rarely glimpse more than the very tip of the
iceberg of the sexual and psychological damage caused by male
circumcision. One symptom is the considerable number of men interested
in foreskin restoration. That any man would be prepared to spend
several hours a day for several years using taped, weighted, and
tensioned devices to try to regrow a foreskin is testimony to the
suffering caused in some cases. In browsing online forums such as www.
restoringforeskin.org, you get a sense of the great missing continent
of male conversations that are unspeakable in public: the Iranian
brought up in the West who always feels something is missing when he
sleeps with a woman, or the gay US man depressed that he does not have
the penis he was born with, like his European lover. Male circumcision
in developed countries is treated simply as a question of opinion. Most
women in the UK do not circumcise their sons, but if a mother says she
has had her son circumcised "to be like daddy" or for "tradition,"
hardly an eyelid is batted.
I was shocked by some comments from mothers, which
seemed more callous than would be tolerated if gender roles were
reversed. In one a mother wrote "LOL" ("laugh out loud") after telling
the forum that her circumcised 4 year old "wants his old penis back."
In another, a mother from South Africa says she has kept the dried
foreskin "in case he wants it back later." Elsewhere on the web, it is
completely acceptable to express a preference for a "cleaner"
circumcised penis on women's sites. I cannot imagine that a man who
advocated ways of making the vagina more "attractive" and "hygienic,"
let alone by surgical means, would be given a moment's hearing.
Legislation to outlaw male circumcision was put
forward in Massachusetts, and although it was defeated campaigns
continue in other states (see www.mgmbill.org). Dutch doctors also
discussed a ban last year (BMJ 2010;340:c2987). A better way to protect
the genitals of young boys might simply be to use existing laws. The
Tasmanian Law Reform Institute has suggested that male circumcision may
breach existing child protection laws (http://bit.ly/eLfxId). And the
media have hinted at the possibility of a test case in the UK (http://
bit.ly/4GviWc). Finally, little boys in the West might be given the
same rights as their sisters, but resistance is peculiarly high and
comes from the most surprising quarters.
Mihail Evans is former postdoctoral researcher in
ethics, University of the West of England mihail@riseup.net Cite this
as: BMJ 2011;342:d978
|
21. Ethical doubts in Turkish journal
|
Turkish Journal of Psychiatry 2014
Ethical Evaluation of Non-Therapeutic Male
Circumcision
M. Cumhur ?sgi MD, PhD, University Lecturer,
Akdeniz University Faculty of Medicine, Department of Medicine History
and Ethics, Antalya, Turkey
SUMMARY
Elective circumcision for nonmedical reasons is a surgical approach
which is historically long standing and accepted as the most performed
procedure. The necessity of the procedure is usually for religious and
traditional reasons alongside some medical ground related benefits to
enable its social acceptability. The discussion of the subject from the
aspect of ethics becomes necessary as there is no consensus about the
benefits or harmfulness of nonmedical circumcision. Fundamental ethical
discussions about circumcision, which
contradicts legal acceptance criteria of any medical application,
are related to the basic concepts of the existence of an individual
such as sovereignty, the loss of
bodily integrity, and privacy. The recent leagal processes
and the fact that the European Council and the American Academy of
Pediatrics have put the issue on their agenda have increased the
necessity of these ethical evaluations. The responsibility of
consideration and evaluation of ethical permission of every
circumcision procedure, besides discussing the necessity of
circumcision for improvement and protection of health rests on the
shoulders of the physicians because the dignity and intellectual
identity of the profession require so.
|
22. Robert Darby powerfully dismantles the "benefits vs
risks" mindset
"Darby offers a vivid critique of our
current justifications for routine male circumcision.
His critique focuses less on the practice itself than on how
we have discussed the ethics of circumcision. He argues that
our analyses of the �risks and benefits� of the procedure have
focused on narrowly medical concerns, and made invisible the
layered symbolic, personal, and psychological significance of
the foreskin and the attendant harms that may result from
removing it without consent. He covers some of the fascinating
social history of our attitudes towards circumcision, and
develops an extended and effective analogy with mastectomy:
while our current practices recognize and incorporate
the potentially powerful personal significance of the female
breast to identity and gender, our circumcision practices have
no such sensitivity. This paper can be difficult to read, as
it can be a challenge to confront a clear-headed critique of a
procedure that many readers underwent or had performed
on their sons with little reflection."
|
23.
Are Physicians Blameworthy for
Iatrognenic Harm Resulting from Unnecessary Genital Surgeries?
(Short answer: Yes, by definition)
|
AMA Journal of Ethics. August 2017, Volume
19,
Number 8: 825-833.
doi: 10.1001/journalofethics.2017.19.08.msoc3-1708.
Are Physicians Blameworthy for Iatrogenic
Harm
Resulting from Unnecessary Genital Surgeries?
Samuel Reis-Dennis, PhD, and Elizabeth
Reis, PhD
Abstract
We argue that physicians should, in certain
cases, be held
accountable by patients and their families for harm caused by
�successful� genital surgeries performed for social and aesthetic
reasons. We explore the question of physicians� blameworthiness for
three types of genital surgeries common in the United States. First, we
consider surgeries performed on newborns and toddlers with atypical sex
development, or intersex. Second, we discuss routine neonatal male
circumcision. Finally, we consider cosmetic vaginal surgery. It is
important for physicians not just to know when and why to perform
genital surgery, but also to understand how their patients might react
to wrongful performance of these procedures. Equally, physicians should
know how to respond to their own blameworthiness in socially productive
and morally restorative ways.
|
24.
Parental authority? No, adult autonomy
|
Jurisprudence
An International Journal of Legal and Political Thought
Volume 8, 2017 - Issue 3
Ritual
male circumcision and parental authority
Kai Moller
Abstract
A
recent judgment by a lower court in Germany brought the problem of
ritual male circumcision to the consciousness of the wider public and
legal academia. This essay weighs in on this emerging discussion and
argues that ritual male
circumcision is not covered by parental authority. It
first considers and dismisses the best interest of the child test,
which is the most widely used test of parental authority in legal
practice. Instead, the essay proposes what it terms the autonomy
conception
of parental authority, according to which parental
authority must be exercised such as to ensure that the child will
become an autonomous adult. While parents may raise their
child in line with their ethical, including religious, convictions,
respect for his autonomy requires that this be done in a way that
allows the child to later distance himself from these values; this
implies, among other things, that irreversible
physical changes are impermissible.
|
i. Voluntary
Amputation forbidden
Voluntary amputations of adults' limbs
"inappropriate"
|
BBC News, February 1, 2000
NO
more private patients suffering from a psychological condition will
have amputations carried out at Falkirk and District Royal Infirmary,
the hospital trust has ruled. Amputations...
Let
me know if this link fails and I will put the whole story
here.
|
ii. Voluntary
Amputation "only if not sexual"
Amputee 'was not sex motivated'
|
Sunday Mirror, February 8, 2000
By JACQUI THORNTON in London
A surgeon in Britain who cut off a man's healthy leg knew that his
patient ran a website for those sexually interested in amputees, The
Sunday Telegraph has revealed.
Robert Smith, a consultant surgeon at Falkirk and
District Royal Infirmary in Scotland, was aware that Kevin Wright was
involved with OverGround, a website which describes itself as "a
support group for people who are attracted to those who have physical
disabilities".
An investigation by The Sunday Telegraph
has revealed that the website is linked to other
web addresses, whose names include Amputees are Beautiful, Fascination,
and Ampix, which includes colour photographs of female amputees.
Other graphics on linked pages include a woman in
black leather fetish wear with one leg amputated above the knee and her
arms around another woman.
However, Mr Wright, who suffers from a rare
pyschiatric disorder, had told Mr Smith that there was no sexual
motivation for the removal of his leg. Instead he believed that he had
an "extra" limb.
The operation was paid for privately by Mr Wright,
but took place in an National Health Service hospital with NHS staff.
He paid $3,500 for the facilities and Mr Smith did not charge a fee.
Mr Smith insisted that he would not have carried
out the operation if a sexual fetish had been a factor.
In an exclusive interview with The
Sunday Telegraph, he denied that he had been "duped" and
said that he was fully aware of Mr Wright's "informative" website" s
contents. He said he was, and is, convinced that Mr Wright had no
sexual reason for the amputation.
He defended Mr Wright's website as an information
provider. "The website Mr Wright started was an information website and
covered the whole spectrum of the problem, although Kevin's own problem
was at the far right of the spectrum, the "need to be's" of those who
want an amputation. At the other far end you have the devotees who are
interested in amputee partners.
"I looked at the website before I decided what I
was going to do and I wanted to make sure that I was dealing with the
right problem. I do not feel I have been duped.
"At the end of the day, I have done the right
thing because the patient is extemely satisfied and has made a major
lifestyle change for the better."
Mr Smith revealed how the patient's wife had
begged him to amputate so that they could lead a "normal life".
The controversial operation, which was followed by
a second on a German patient two years' later, has caused widespread
protest, and Dennis Canavan, the Labour MP, has called for an inquiry.
He said: "I find it almost incredible that a
reputable surgeon would amputate a perfectly healthy limb. The
existence of the website raises grave concerns."
Mr Smith said last week that he believed his
patient was no longer involved with OverGround. However, Mr Wright's
name and address was printed as the contact for more information before
the site was clsoed. The surgeon admitted that the condition was
"incomprehensible" to him, and that he was extremely apprehensive at
the start of the operation, but was ultimately "gratified" by the
excellent result.
He has kept in touch with both amputees, Mr Wright
who was operated on in 1997 , and the German patient who he operated on
last year who asked for help through Mr Wright.
Mr Smith said both were "delighted" by the results
of the above-the-knee amputation, which they had specifically requested.
"There has been an absolute change in their lives.
As soon as they knew they were getting the operation their demeanours
and attitudes changed," he said."Curiously, they seem more active than
they were before, they are more interested in life and their lives are
much happier."
Mr Smith said that two pyschiatrists and a
psychologist had already assessed Mr Wright, and they confirmed that he
was suffering from a form of Body Dysmorphic Disorder called
Apotemnophilia, which has two forms. The first group fantasises about
being an amputee as a form of sexual arousal.
The second group, of which he said Mr Wright was a
member, regards their body as incomplete with four limbs but complete
after amputation, and who always wanted the same limb amputated. He
added that this group was a very small sub-section of Apotemnophiliacs
and would injure themselves to achieve amputation.
He said: "It is part of their daily life. They
imagine themselves as an amputee going along the street shopping. It's
not just during sexual activity. The last people you want to operate on
are those who are doing it for sexual arousal."
Mr Smith said that after 18 months he decided to
accept Mr Wright as a patient having discussed the issue with the
hospital's medical director, the chief executive, the General Medical
Council and the Scottish Medical Defence Union.
The British Medical Association said Saturday that
their Ethics Committee was not investigating the case. A spokesman
said: "We do not look at individual cases like this."
But he added: "This surgeon thought long and hard
about this, for 18 months in fact, and considered all the psychiatric
reports before he came to his decision."
Mr Smith said that the patient came for a
consultation with his wife. "We had a long discussion about the
problem. He explained that he had this feeling for most of his life
that he should be an amputee, he really only had one leg, and he wanted
the leg removed. He had had considerable problems over the years, a
very troubled life and psychiatric treatment which had not solved the
problem.
"His wife was saying: 'I wish to God someone could
take his leg off and then we can lead a normal life.'
"I ultimately became convinced that this was
really the only way in which we could attempt to resolve the problems."
He said Mr Wright was even happier it had come out
in the open. "He doesn't have that fear hanging over him that he's
going to get found out," he said. The hospital trust where it was
carried out, Forth Valley Acute Hospital NHS Trust , banned the surgery
last year after an internal inquiry. A spokesman declined to comment on
the revelation that Mr Smith had known about his patient's involvement
in websites.
"For reasons of medical confidentiality, we never
discuss an individual patient's case. If Mr Smith has decided to
comment that is a matter for him."
Mr Wright, a teaching assistant at the University
of Essex, England, would only say that he regarded the operation a
"private and personal medical matter."
The OverGround website was closed down on
Wednesday, the day after news of the operation broke."
Since the publicity, two partners of
apotemnophiliac men have contacted the surgeon asking for advice. A
further two patients have been assessed and were waiting for surgery
when the hospital banned the operation.
Some experts believe that amputation can
exacerbate the problem because it increases pre-occupation with the
imagined defect.
- The Sunday Telegraph
|
[The
striking thing about this story is the high level of concern shown by
doctors for the mental health of a person wanting to have one of his
own limbs cut off (and rightly so). A sexual reason would
have instantly disqualified Mr Wright from having his leg amputated.
Yet doctors such as Williamson and
Williamson viewed with equanimity, even approval, women who
wanted to have part of their sons' genitals cut off to suit their
sexual tastes.]
iii. Voluntary
amputation "unethical and we wouldn't do it"
|
The Dominion Post (New Zealand), June 23, 2005
'I
need to remove my leg in order to feel whole'
|
|
� AUSTRALIA
SURGEONS should be
allowed to cut off the healthy limbs of some "amputee wannabes", two
Australian philosophers believe.
Neil Levy and Tim
Bayne argue that patients obsessed with having a limb amputated should
be able to have it safely removed by a surgeon, so long as they are
deemed sane. ...
But vascular surgeon
John Quinn said removing a normal limb would be considered unethical in
Australia.
|
There are some people who've got psychiatric
disorders who want all sorts of things done," said Dr Quinn, the Royal
Australasian College of Surgeons' executive director of surgical
affairs.
"It's different than removing normal kidneys for
transplantation, which has a different purpose and it's helping
different people. But to remove a normal limb because somebody thinks
it would be a good thing is unethical and we wouldn't do it."
AAP
|
[And the
difference from infant circumcision is? "The foreskin is not a limb."
And the significance of that is what? Echo answers "What?"]
iv. Ethics of
taking umbilical blood
The blood from a baby's umbilical cord is a rich source
of haematopoeic [blood-making] stem cells, which can give rise to any
of the blood's valuable components. They are especially valuable in
treating leukaemia. Cord blood is storable and more likely to be
compatible than bone marrow.
The April 2001 edition of Scientific American pays
particular attention to the ethics of using one baby's umbilical
stem-cells in another person - even though the baby would in all
probability have no use for them him/herself. The front cover reads:
|
 Whose Whose
 Blood Is It, Blood Is It,
 Anyway? Anyway?
 CORD STEM CELLS SAVE CORD STEM CELLS SAVE
|
 LIVES BUT RAISE QUESTIONS LIVES BUT RAISE QUESTIONS
|
And the story includes:
... the doctor usually tosses it into a
stainless steel bucket with the rest of the medical waste bound for
incineration.
But more and more physicians and parents are realising the value of
what they used to regard as merely birth's by-product. ...
But like many new scientific discoveries, umbilical cord blood
transplantation brings with it a set of ethical questions. [see
box on next page]. Who owns umbilical cord blood: both
parents, the mother or the infant? What happens if a mother donates her
baby's cord blood to a bank but the child later develops leukemia and
needs it? The ethical questions are compounded by the advent of
for-profit companies that collect and preserve a newborn's cord blood
for possible use by the family later.
|
- followed by this sidebar:
|
But Is It
Ethical?
Marketing
tactics and privacy issues raise eyebrows
LAST SEPTEMBER, a little girl...received a lifesaving transplant of
umbilical cord blood from her newborn brother, Adam....Was this
ethically appropriate? A panel of bioethicists decided that it was,
because donating cord blood would have no effect on Adam's health.
...Questions have been raised in the past concerning the ownership of
cord blood. But bioethcist Jeremy Sugarman of Duke University states
that it is now fairly clear that although an infant owns his or her own
cord blood, parents have legal guardianship over it - just as they do
over the child - until he or she reaches the age of 18.
|
One interesting thing about this article is the parallel
between the ethics of taking a baby's umbilical cord blood (which s/he
will almost certainly never need) and taking his foreskin (which the
great majority of intact men value highly), and its sale and use by
other people.
Another is the immediate concern shown with the ethical
issues of this brand new (and so far tiny) area of medicine, compared
with the deafening silence about - and refusal to consider - the
ethical issues raised by infant circumcision.
v. How a Christian
ethicist reconciles faith and ethics
|
One of the challenges of being a Christian who
does ethics in a secular medical setting is struggling with how to
integrate your own personal beliefs in a setting where overt religious
and theological considerations really aren�t considered appropriate,
unless they are the patient�s or family�s religious beliefs. What I�ve
discovered is that where my religious beliefs take me is rarely
different from where a standard bioethics analysis might take me. And,
I think one of the skills I�ve had to learn is that if I do arrive at a
decision about what I think is the right thing to do and my reasons for
believing that are related to my religious beliefs, I have to be able
to craft secular arguments to support that view. [Isn't the
ethical way of working, to work out from the facts and
ethical principles what is right and wrong, and if religion says
otherwise, to critique that religion?] The real art of
bioethics is convincing other people why something is right or
something is wrong and why something shouldn�t be done or should be
done. [Isn't the best way to do that, to have a convincing
ethical argument?] Many people aren�t
going to pay attention to you if that argument
is crafted purely in religious language. One of the things that I�ve
had to do is craft arguments in the language of the world, which I have
not found to be particularly difficult. The reality is that medical
ethics has its roots largely in theological ethics, so the basic
principles that many people who are not religious subscribe to actually
have very strong roots in the Bible and in religious belief.
- Dr Douglas Diekema in the Calvin College Spark Winter 2007
Dr Diekema is
ethicist at the Children�s Hospital and Regional Medical Center in
Seattle. He led the ethics panel that agreed that a severely disabled
girl identified as Ashley should have hormones, a hysterectomy and
breast-bud removal to prevent her ever maturing.
He was chair of the AAP Bioethics Committee that in 2010 recommended allowing
a token ritual nick to girls, "much less extensive than male
genital cutting" (until public outcry made it back down).
And he was ethicist to the 2012 AAP Task Force on Circumcision.
|
Related pages:
Back to the Intactivism index
page.
|
|
